By Sam O’Brien
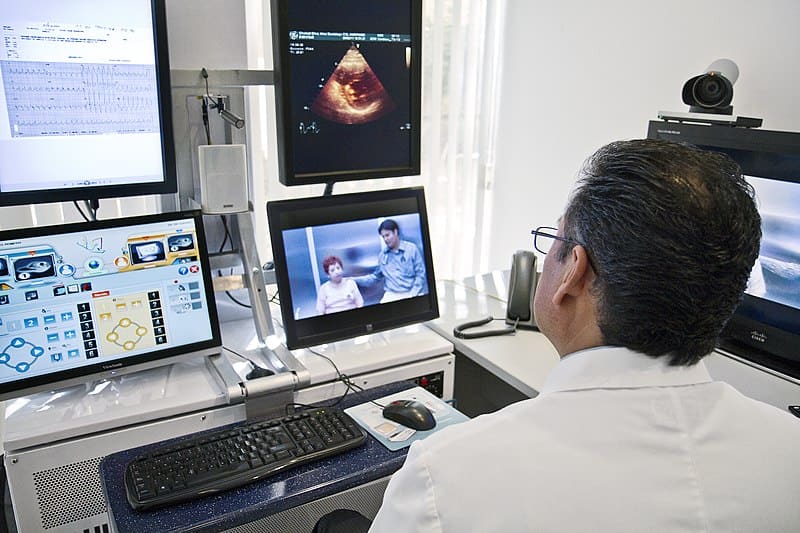
In recent years there’s been a revolution gaining pace in healthcare. The advent of online meeting platforms for telemedicine courses has changed the way that healthcare services are delivered, allowing patients to seek consultations from the comfort of their own home. This saves patients from the hassle of trekking out to a GP surgery, clinic or hospital for face-to-face consultation.
While telemedicine was already being widely touted as the future of healthcare before the pandemic, the onset of Covid-19 has seen a notable increase in take-up of the technology. Some doctors, keen to keep people out of surgeries, clinics and hospitals (all environments where the virus is particularly liable to spread) have sought to offer remote consultations instead.
Unfortunately, there is no indication that the virus is going to disappear any time soon. This has forced us to make big, and quite rapid, changes in a number of areas. We’ve had to change the way we work and communicate; technologies such as video conferencing have helped businesses to maintain at least some semblance of normality, and having creative virtual backgrounds for Zoom put some levity to the situation.
It stands to reason that similar technologies might be used to deliver healthcare services remotely. For all the focus on Covid-19, it’s also important to remember that people are still falling ill or experiencing other health problems at the same time. It’s essential to ensure that they’re getting the help they need, when they need it – without putting them at additional risk to do so.
Both private insurance firms and government healthcare programmes are starting to utilize these numerous well-established telemedicine services and authorized telehealth medical certificates more as often. In the years ahead, we can expect that adoption of telemedicine will grow further. Patients and providers will get more used to the technology and better understand what it can do.
If you’ve never used a telemedicine service such as telemedicine for diabetes, you might be a little unsure as to what it’s all about. Perhaps you’re a bit apprehensive about whether it can provide you with the standard of care you expect. In this concise guide, we’ll explain more about what telemedicine is or what is virtual PBX? what it’s for and what its potential benefits can be.
One thing it’s important to remember is that telemedicine is not intended to totally replace face-to-face care. It can help to lighten the load on healthcare systems, as well as saving you unnecessary hassle. People can access consultations via live web chat more quickly, and do so without having to travel.
Here, we’ll give you a quick but comprehensive introduction to telemedicine, its history, and what it might mean for you. First of all, we’ll start by answering that all-important question – what is telemedicine?
What is telemedicine?
There is still some confusion about the distinction between telemedicine and telehealth. The two terms are often used interchangeably, which tends to confuse the matter further. Telehealth is an umbrella term used to cover the use of telecommunications and information technologies to support healthcare provision. It also includes remote public health and healthcare education, and administrative functions.
The term ‘telemedicine’ specifically refers to the provision of healthcare to patients via remote means, such as video link. As we’ve noted, video conferencing is becoming increasingly commonplace, especially since the onset of the pandemic. So too is the remote provision of healthcare services, as practitioners seek to limit face-to-face contact.
While telemedicine has grown at a remarkable rate, most patients still have little experience of using it. However, the initial uncertainty that many patients once felt is dissipating. It appears that more people are willing and prepared to make use of telemedicine services. Since Covid-19 swept the globe, it has made sense for top telemedicine providers to scale up their services and help restrict the spread of the virus.
There are three primary types of telemedicine: interactive voice response meaning in medicine (which is where patients and practitioners communicate remotely in real time, i.e. via a video calling), store and forward (where physicians and providers share patient information with others), and remote patient monitoring (where data is collected to monitor patients’ conditions).
It’s probably fair to say that most people associate telemedicine with the first aspect: interactive medicine, and remote consultations with doctors. In previous years, such consultations would have generally been laggy and unreliable. Recent advances in broadband connectivity and personalizing websites to boost page speed have made it possible to hold remote consultations via the internet while ensuring reliability and clarity.
As a result, telemedicine is now commonly used in the treatment and monitoring of a wide range of conditions. These include asthma, cold and flu, arthritis and bronchitis, as well as common sprains and strains. Anything that doesn’t need a physical examination can easily be moved to personalized recommendations online. They can also be used for follow-up discussions after an operation or chemotherapy, or to talk patients through their test results.
Of course, the type of telemedicine used in a patient’s treatment will depend both on their personal condition and the healthcare provider they’re using. Patients who want to make use of telemedicine should speak to their doctor or provider. They’ll be able to provide more information about the technology, the uses to which it is put and the appropriate EDI (electronic data interchange) security measures in place.
Don’t worry about whether you’ve got the exact terminology right, either – whether you call it a remote appointment, telemedicine or telehealth, your doctor or healthcare provider will know what you mean.
A brief history of telemedicine
There’s been a lot of discussion over the last decade about telemedicine and the transformative impacts it might have on healthcare provision. The technological revolution of recent years has encompassed everything from AI in call centres to robotic surgeons. The saturation of mobile technology makes it possible to roll out saas products and services to patients in a way that wasn’t an option before.
You might not realise that telemedicine has a much older heritage. In fact, the original telemedicine founders were a range of healthcare and educational institutions working in the mid-20th century. Arguably the first prototype of telemedicine emerged in 1925, when inventor Hugo Gernsback proposed the ‘teledactyl’ – a device which would have remotely examined patients while relaying a video feed.
The next major step towards what would become known as telemedicine came in 1959 at the University of Nebraska. This introduced a two-way interactive television system, used to transmit images of neurological examinations so that students could monitor them remotely. By 1964, a link to the Norfolk State Hospital (112 miles away) had been established, and was used to help provide a range of services.
At this early stage in its development, the main potential of telemedicine lay in its ability to reach patients in rural districts of the United States. These patients, who would otherwise lack access to specialists, suddenly had access to a broader range of medical professionals. The technology could also speed up the provision of treatment and cut down on waiting times by facilitating quicker sharing of test results and patient records.
Telemedicine continued to evolve at an accelerated rate through the 1960s and 1970s. A plethora of US government agencies and public bodies – including Nasa and the Pentagon as well as healthcare departments – showed increasing interest and invested large sums of money into further development.
More recently, telemedicine has come to play an increasingly prominent role in our everyday lives. Many of us even may not even realise just how pervasive it has become. Of course, there’s the rise of mobile global app testing which we can use to arrange consultations with GPs or arrange repeat prescriptions. But the reach of telemedicine extends further.
In fact, you probably have a telemedicine app or device yourself. Wearable fitness trackers wearables are very popular, making it easier for people to monitor and check a range of health data. These might include heart rate monitors, wristbands or smartwatches. Your mobile phone probably has an app that tracks your daily step count.
Taking all this into account, you can see just how far telemedicine has come within the space of a few decades. Consider just how many of us have mobiles, tablets and laptops, and how accessible this makes telemedicine services as a result. It seems a safe bet that usage of remote medical services is only going to increase in the years ahead.
How telemedicine can benefit patients
We’ve heard a great deal about the potential benefits telemedicine might have. The technological changes we’ve seen have been so far-reaching that it seems safe to assume that telemedicine technology is only likely to grow further in the coming years. But what exactly will this mean for patients?
As we’ve already noted, Covid-19 has had transformative effects of its own on the delivery of healthcare. Until we have a vaccine for the virus, we’re all going to have to take certain precautions to limit its spread. One of these is accessing more services remotely rather than in person. Medical provision is one of these; while there are forms of care that have to be carried out face-to-face, others can be done remotely, and quite easily.
This is the most obvious benefit telemedicine can have for patients at the moment. It can help to keep them safe from Covid-19, saving them from taking the risk of attending certain kinds of appointments in person. The virus can easily circulate in surgery and hospital waiting rooms, so the less time people spend in these, the better. It also reduces the amount of people in waiting rooms, so those who can’t make use of telemedicine still share in the benefits.
Another point that’s important to remember is that many people have mobility issues. This can make it challenging to attend a doctor’s appointment in person. This is even more obvious if they have to attend a surgery, clinic or hospital that’s further away. It may not always be practicable for general practitioners to make home visits, as their time is limited. Specialists will cover a large area, making it even more impractical.
Telemedicine can therefore serve as a more convenient alternative for both patients and practitioners, allowing the former to be seen, while also making it easier for the latter to fit them into their own busy schedule. This can be particularly valuable for disabled and elderly patients, as well as those who have suffered some sort of physical injury.
Another upside to the increased adoption of telemedicine services is that it could help to ensure stretched healthcare budgets go that bit further. There’s been a concerted squeeze on health expenditure in many countries around the world. The effects of this have made themselves apparent in the form of longer waiting times and cuts to certain services.
Telemedicine could help to ease some of the strain on these budgets by freeing up financial resources that might otherwise have been used less efficiently. So long as budgets and services aren’t scaled back further, this could help to deliver improvements to the quality of small business phone service provision at the same time as enhancing overall efficiency.
It may also force healthcare providers to reconsider the standards of care they offer to patients. The immense choice offered by the internet has forced many businesses to reconsider a crucial question: namely, what is world class customer service? It could be that healthcare bodies are compelled to ask themselves a similar question as telemedicine grows in popularity and reach.
Conclusion
Technological advances have forced us to revisit many of our prior assumptions over the last few years. They’ve also opened up a world of choice that previously wasn’t open to us. Not only has it given us more options in finding, say, the best call center software, or the most up-to-date smartphone, but it’s provided us with a huge range of choices elsewhere as well.
It stands to reason that this would also come to include healthcare as well. Of course, healthcare is never quite as straightforward as being a simple consumer – as lay people our ability to make informed choices is more limited. Patients also want to be treated as something more than just a customer when we need treatment for whatever reason. Nevertheless, the quiet revolution in telemedicine is changing the way healthcare is provided.
The most important benefit telemedicine could have is simply allowing us to lead better, healthier lives for longer. It could enable people to lead richer lives, with a better quality of life, where otherwise they may struggle to obtain the specialist help they need. That’s something that seems more important than ever at a time like this.
About the Author

Sam O’Brien is the Senior Website Optimisation & User Experience Manager for EMEA at RingCentral, a Global VoIP, video conferencing and cloud PBX for Microsoft Teams software provider. Sam has a passion for innovation and loves exploring ways to collaborate more with dispersed teams. He has written for websites such as G2 and Hubspot.
Disclaimer: This article contains sponsored marketing content. It is intended for promotional purposes and should not be considered as an endorsement or recommendation by our website. Readers are encouraged to conduct their own research and exercise their own judgment before making any decisions based on the information provided in this article.